By Miranda Spindt
Vice President Kamala Harris will be in Wisconsin on Monday touting new federal staffing requirements for federally-funded nursing homes. But while the Biden Administration has identified a very real problem, their preferred solution is likely to only make things worse for families struggling to find affordable facilities for seniors. First, a little context on the problem.
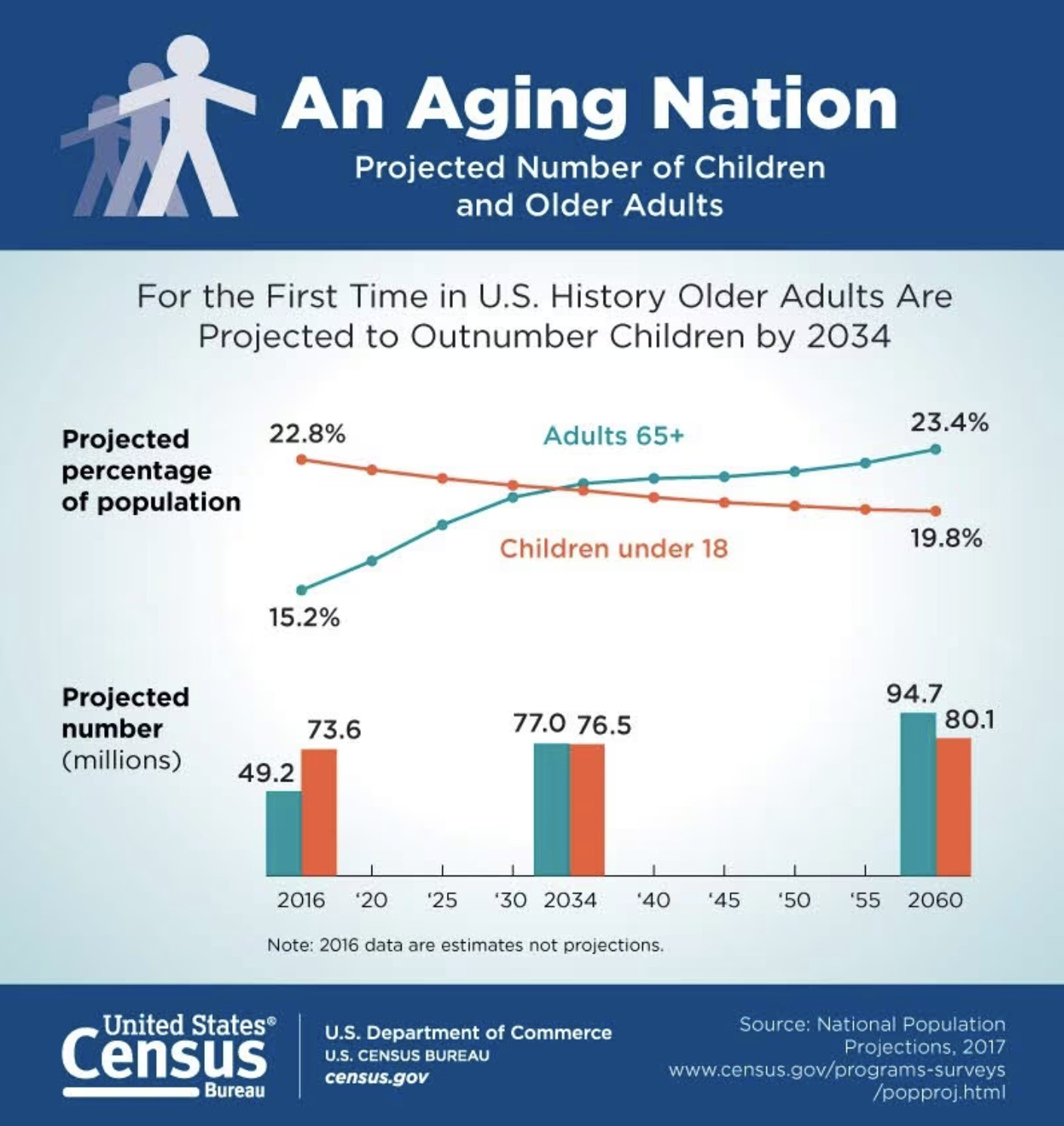
Medicaid provides long-term care services for eligible seniors1-covering 100% of the costs– and making up 32.1% of all Medicaid spending. Long-term demographic changes have put the future of this program in jeopardy. By 2030, everyone in the Baby Boomer generation will reach the age of 65 and, for the first time in history, seniors are projected to outnumber children under the age of 18 by 2034. This means there will be fewer working adults to care for the higher number of seniors. With long-term care facilities struggling to find staff, we are already seeing the consequences.
In Wisconsin, 60 nursing homes have closed since 2016 largely due to a shortage of Certified Nursing Assistants. A study from 2022 highlights some troubling statistics about the future of the long-term care workforce in Wisconsin.
- The number of unfilled caregiving positions in nursing homes and other elderly care employment was 12.9% in 2016. In 2022, that was more than doubled at 27.8%. That includes certified nursing assistant positions with a vacancy rate of 28.4%.
- The COVID-19 pandemic hit healthcare employment hard, but long-term care facilities have not recovered as well as other sectors such as hospitals and clinics due to having the strictest COVID-19 safety requirements, and inability to compete with private sector employee pay and benefits.
- As the elderly population rises shown in the image below, there is a projected gap of 19,800 registered nurses by 2040 in the long-term care sector.
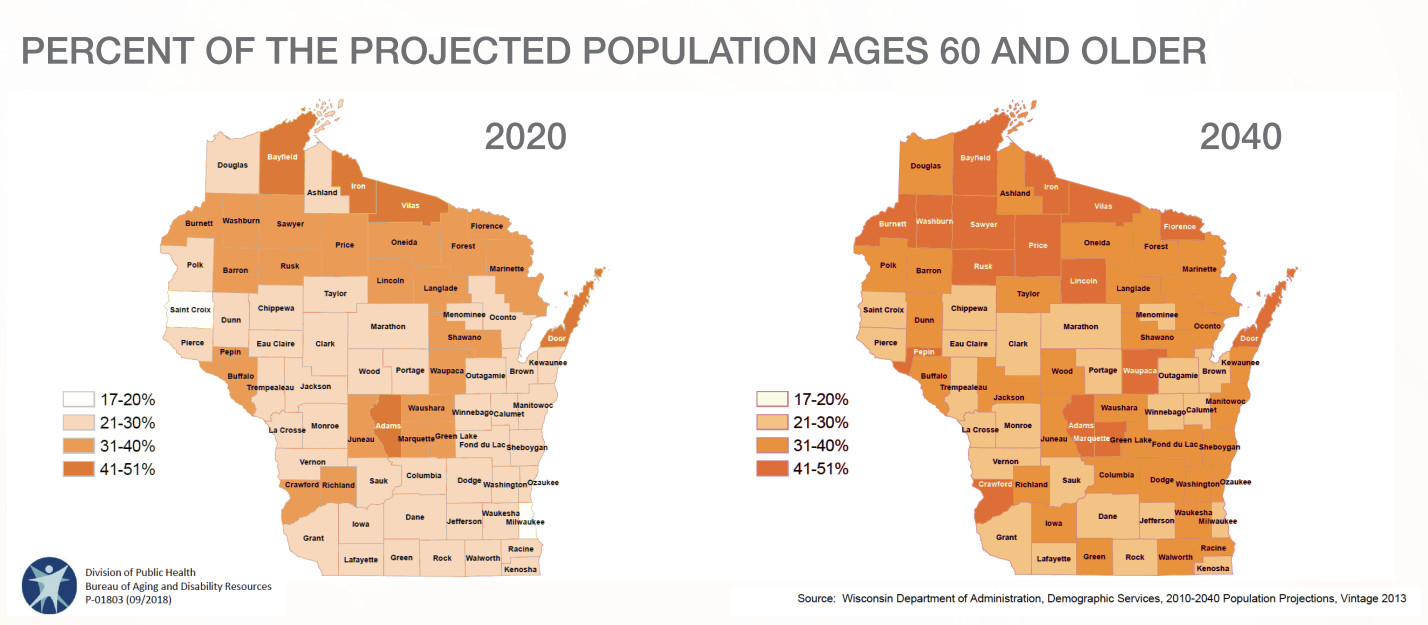
The quality of care suffers as facilities are understaffed and employees are overworked. The number of complaints against nursing homes has been rising in recent years as the staffing shortage has worsened. This is especially problematic in rural areas where older adults are a higher share of the population compared to urban or suburban areas, and they already struggle finding workers in multiple healthcare sectors with many counties designated as Health Professional Shortage Areas for primary, dental and mental care.
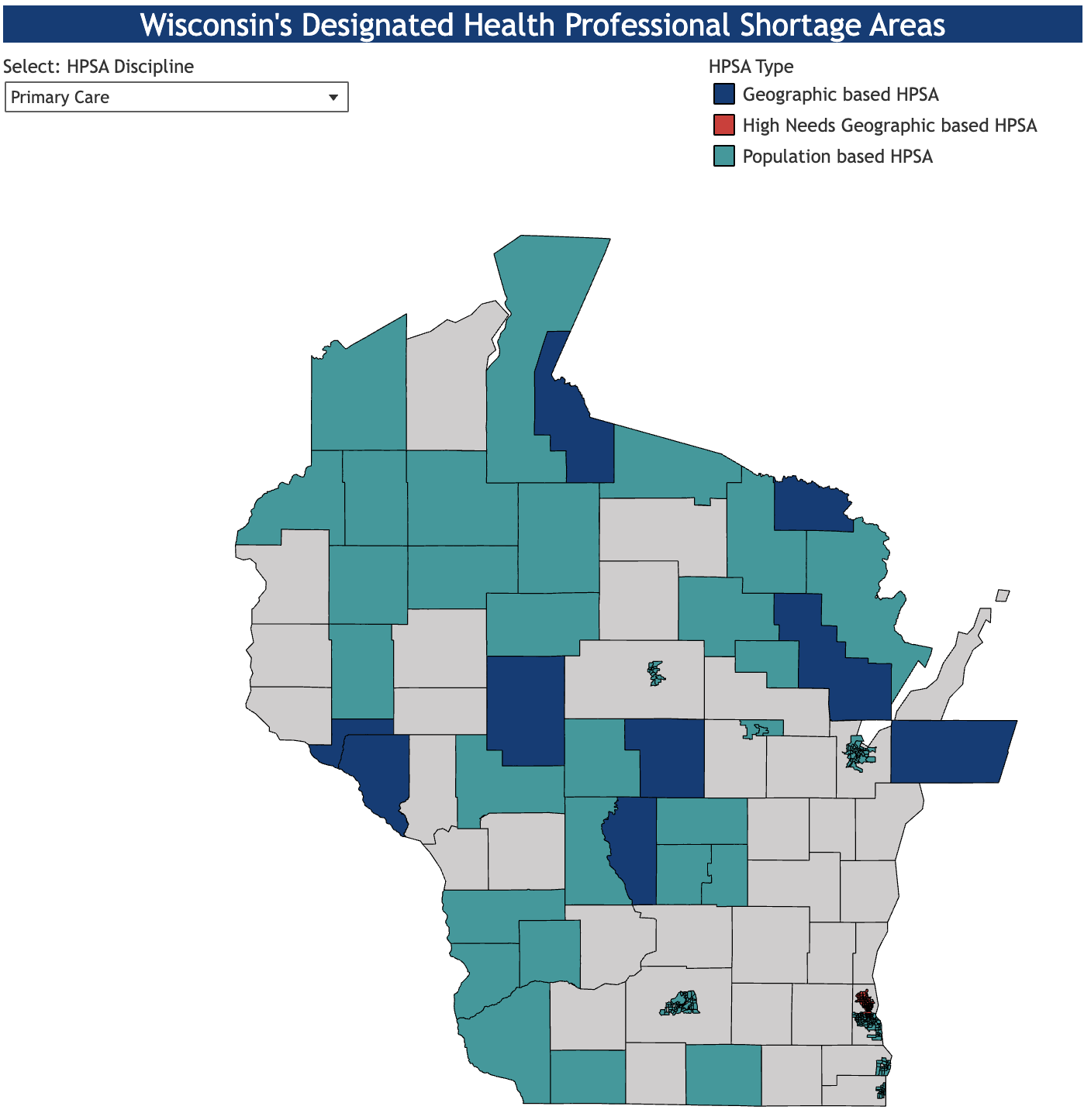
The Biden Administration proposed a rule last September that would require minimum staffing levels at to attempt to improve the quality of long-term care. But like most well intentioned federal government rules, this could actually have the exact opposite effect. The rule would require a registered nurse to be on-site 24 hours a day, and for each resident, there must be 33 minutes of registered nurse care and 147 minutes of nurse aid care each day. This means that a facility with 100 residents and 8-hour shifts must be staffed with two or three registered nurses and about ten nurse aides each shift. If this rule is passed, 3 in 4 facilities in Wisconsin would be forced to hire additional staff or shut down entirely if they can’t meet those standards.
While this proposed rule could spell disaster for nursing homes, Wisconsin has options to improve the pipeline of nursing aides working in long-term care facilities, thus raising quality without ruining the industry. Currently, Wisconsin requires Certified Nursing Assistants (CNA) to complete 120 hours of training before they can enter the workforce. The federal government only requires states to have 75 hours of training, a standard that 19 states follow, including our neighbors Michigan, Minnesota and Iowa. The additional hours put Wisconsin at a regional disadvantage and pose a barrier to entering the field because it complicates the hiring process and adds to the overall cost of training. In 2019, the legislature introduced AB 76 which would have reduced the required hours to 75 hours, bringing Wisconsin in line with our neighboring states. However, Governor Evers vetoed the legislation.
Ironically, in 2020, Governor Evers issued an emergency order to encourage more people to become CNA’s during the pandemic which included reducing the minimum number of training hours from 120 to 75, and he even had over 200 national guard members trained as CNA’s during this time. Unfortunately, this rule was withdrawn on June 6th, 2022. This begs the question, why were reduced training
hours okay during the height of the pandemic, but not okay afterwards?
It’s important to note that aligning the training standard with the federal requirement does not compromise the quality of training or care provided. CNA’s would still undergo training in eight subject areas, and facilities catering to specialized patient populations can provide additional training as needed. Moreover, the proposal does not mandate changes to existing CNA training programs; those wishing to offer more than the federal standard are free to do so.
Looking at Minnesota, Michigan, and Iowa, which require 75 hours, there are several quality measures that they outperform Wisconsin. Compared across nine quality measures, at least one of these other states outperforms Wisconsin in seven of them. This shows that the number of minimum hours is not a determining factor of quality care. As more people seek the chance to become a CNA and enter the workforce sooner with fewer training hours, quality issues stemming from staffing shortages will be alleviated.
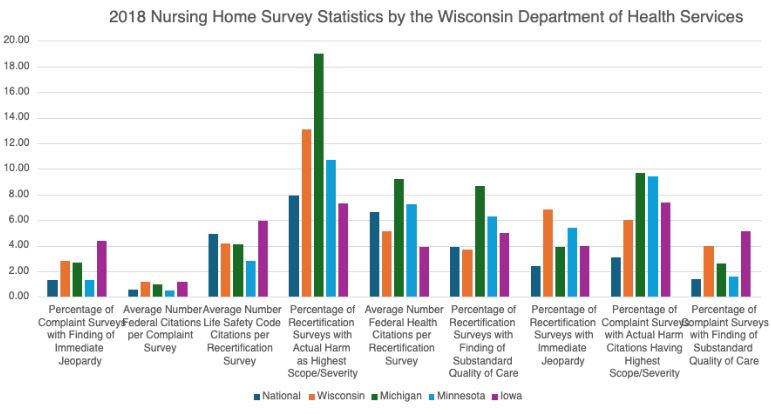
This is not the only solution to addressing the issues we face with Medicaid and long-term care as our population ages. However, the alignment of training requirements is seen as a crucial step in addressing Wisconsin’s workforce crisis to strengthen the nurse aid pipeline and ensure residents receive the quality care they deserve.